Venous leg ulcers can significantly impact your quality of life, causing discomfort and hindering mobility.
If you or a loved one are living with a venous ulcer, we are here to help.
At Tennessee Vein Center, we understand the challenges of venous leg ulcers and offer specialized treatment options to address this condition effectively.
Here, we delve into venous leg ulcer treatment, exploring its symptoms, causes, and various therapeutic approaches to promote healing and restore wellness. Continue reading to learn more.
What is a Venous Leg Ulcer?
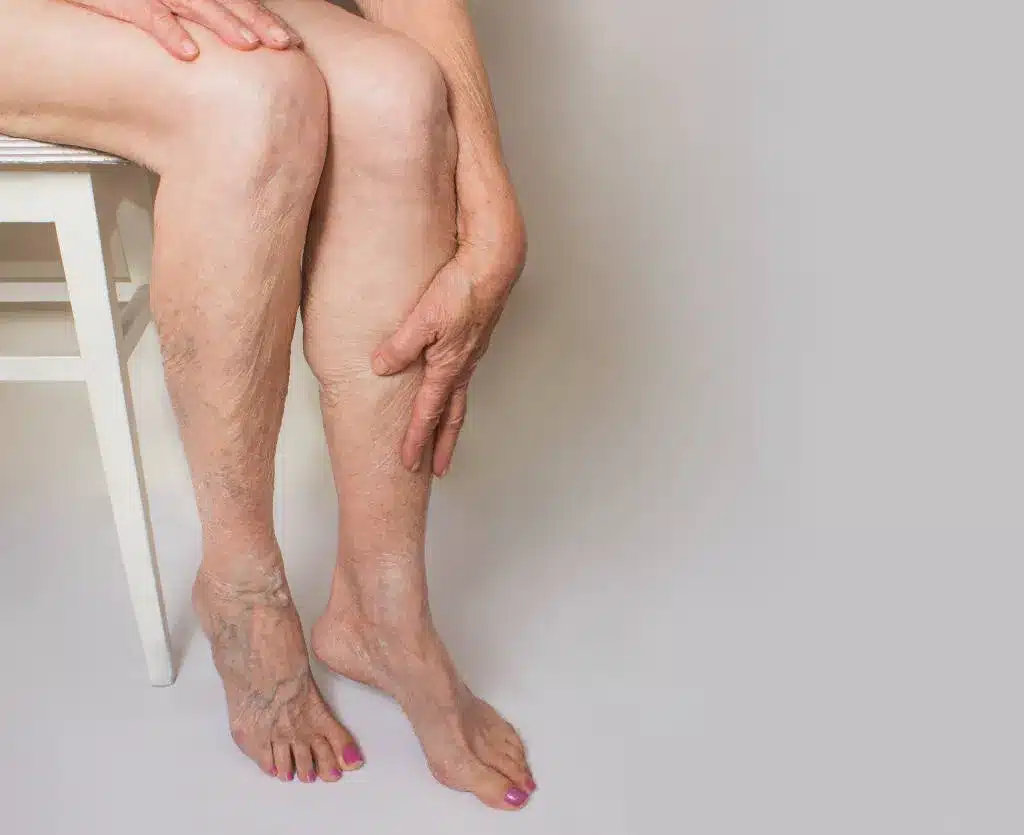
A venous leg ulcer is an open wound that develops on the lower legs or ankles due to chronic venous insufficiency. This condition occurs when faulty vein valves impair blood flow, leading to increased pressure in the veins and subsequent tissue damage.
Leg Ulcer Causes
There are several types of leg ulcers, each with distinct characteristics and underlying causes.
Some common types of leg ulcers include:
Venous Leg Ulcers: These are the most common type of leg ulcers and are typically caused by chronic venous insufficiency. Venous leg ulcers often occur near the ankles and are characterized by shallow, irregularly shaped wounds with surrounding skin discoloration and swelling.
Arterial (Ischemic) Ulcers: Arterial ulcers develop due to poor blood circulation in the arteries, often due to peripheral arterial disease (PAD). These ulcers are commonly found on the feet or toes and are characterized by deep, painful wounds with well-defined edges. The skin surrounding arterial ulcers may appear pale or bluish.
Neuropathic (Diabetic) Ulcers: Neuropathic ulcers are a complication of diabetes and occur due to nerve damage (neuropathy) in the legs and feet. These ulcers typically develop on weight-bearing areas of the foot and are characterized by shallow, painless wounds with calloused or thickened skin around the edges.
Mixed Ulcers: Some leg ulcers may have characteristics of more than one type, such as a combination of venous and arterial insufficiency. These mixed ulcers require comprehensive assessment and treatment addressing both underlying causes.
Pyoderma Gangrenosum is a rare type of ulcerative skin condition characterized by rapidly progressing, painful ulcers with undermined edges. Pyoderma gangrenosum ulcers may occur anywhere on the body, including the legs, and are often associated with underlying immune system disorders.
Identifying the specific type of leg ulcer is crucial for determining the most appropriate treatment approach. Proper diagnosis and management by a healthcare professional, often in collaboration with a wound care specialist or vascular surgeon, are essential for promoting healing and preventing complications.
Leg Ulcer Causes
Leg ulcers can have various underlying causes, which may include:
- Chronic venous insufficiency: One of the most common causes of leg ulcers. It occurs when the valves in the leg veins malfunction, leading to poor circulation and blood pooling in the lower extremities. Over time, this can result in tissue damage.
- Lipodermatosclerosis is a chronic condition characterized by inflammation and fibrosis of the skin and underlying tissues of the lower legs, often associated with venous insufficiency.
- Venous stasis dermatitis, also known as stasis dermatitis or gravitational eczema, is a skin condition that occurs due to chronic venous insufficiency. It is characterized by inflammation, redness, itching, and skin scaling, usually affecting the lower legs and ankles.
- Atrophie blanche is a skin condition characterized by ivory or white-colored patches, typically occurring in individuals with chronic venous insufficiency and often associated with underlying damage to the blood vessels and tissues.
- Arterial disease: Peripheral arterial disease (PAD) causes narrowing or blockage of the leg arteries, leading to reduced blood flow to the tissues. Inadequate blood supply deprives the tissues of oxygen and nutrients, increasing the risk of ulcer formation.
- Diabetes: Individuals with diabetes are at higher risk of developing leg ulcers due to various factors, including neuropathy (nerve damage), peripheral vascular disease, and impaired wound healing.
- Trauma or injury: Direct trauma or injury to the skin, such as cuts, burns, or surgical wounds.
- Infection: Bacterial, fungal, or viral skin infections can contribute to the development of leg ulcers, mainly if left untreated or if the individual has a weakened immune system.
- Certain autoimmune conditions, such as vasculitis or pyoderma gangrenosum.
- Lifestyle factors such as obesity, smoking, and a sedentary lifestyle.
- Chronic medical conditions, including hypertension, heart disease, kidney disease, and certain types of cancer.
Venous Ulcer Symptoms
Leg ulcer symptoms may include:
- Varying degrees of pain, ranging from mild discomfort to severe throbbing or aching sensations in the affected area.
- Swelling of the legs, ankles, and feet
- Discolored skin around the ulcer often takes on a reddish-brown or purplish hue due to poor circulation and blood pooling in the affected area.
- Itching or burning sensations in or around the ulcer site.
- Drainage or oozing can range from clear fluid to yellow or greenish pus, depending on the presence of infection or other complications.
- Skin texture changes, such as becoming dry, scaly, or hardened (lipodermatosclerosis) or taking on a shiny, tight appearance.
- Slow healing.
- An unpleasant odor due to bacterial colonization or infection.
It is important to know that elevating the affected leg above heart level may worsen pain or discomfort due to increased venous pressure and blood pooling in the veins.
If left untreated, venous ulcers can lead to complications such as cellulitis (skin infection), osteomyelitis (bone infection), or even sepsis (systemic infection), which can cause fever, chills, and general malaise.
It is essential to seek medical attention from a leg ulcer doctor if you experience any of these symptoms, as prompt treatment is crucial for preventing complications and promoting the healing of venous ulcers.
Venous Ulcer Treatment Options
Our experienced team specializes in providing a range of effective treatment options for leg ulcers.
Accurate diagnosis is crucial for effectively treating venous ulcers and is the first step in addressing any vein disease condition.
Under the expert care of Dr. Campbell, who has been treating venous ulcers and related venous issues since 2003, you can trust that your condition will be evaluated appropriately.
Medical consultation and duplex venous ultrasound are the initial steps to diagnosing any venous problem, allowing us to determine the cause of the ulcer and recommend the best vein treatment option for you.
Once a proper diagnosis is made, addressing the underlying cause of venous ulcers is essential. Treatment typically involves sclerotherapy and endovenous thermal ablation to target the vein disease as soon as possible.
A recent study published in the New England Journal of Medicine recommends immediate treatment of venous ulcers for quicker healing time. These treatments have been shown to reduce healing time by as much as 50% and decrease the likelihood of recurrence.
In addition to medical interventions, lifestyle modifications can also improve venous health. Regular exercise, leg elevation, wearing compression socks, and avoiding prolonged sitting or standing are all beneficial practices for managing and preventing leg ulcers.
How Venous Leg Ulcers Are Diagnosed
Accurate diagnosis is the foundation of effective venous leg ulcer treatment. While the ulcer itself is visible, determining why it formed is essential for proper healing and long-term prevention.
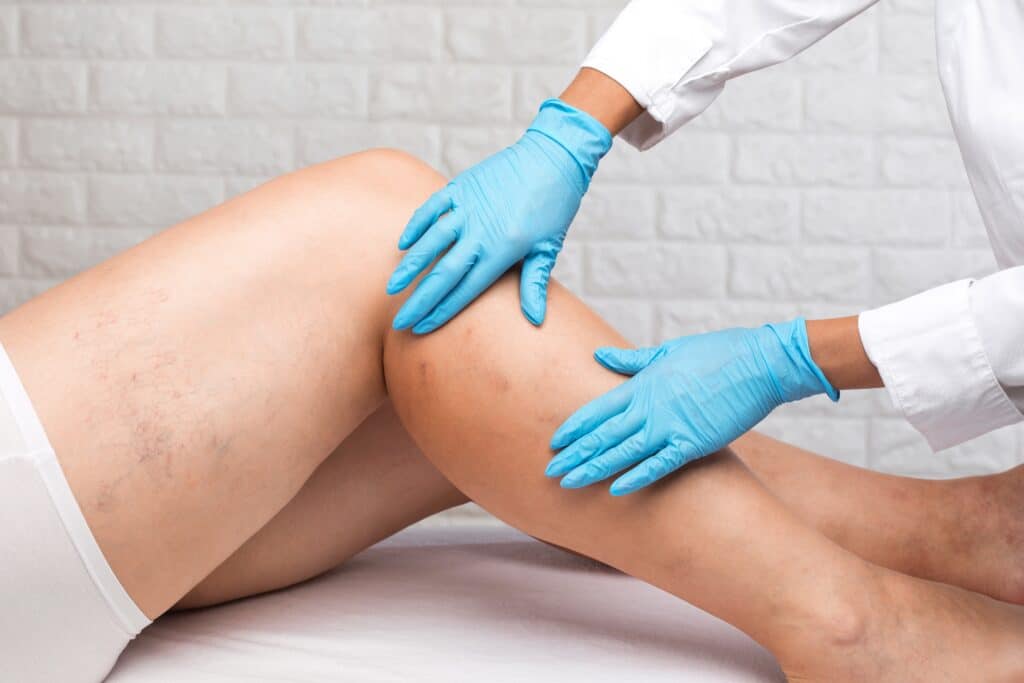
Diagnosis typically begins with a thorough medical history and physical examination. Your provider will evaluate the location of the ulcer, surrounding skin changes, swelling, and any history of vein disease, blood clots, or prior ulcers.
A duplex venous ultrasound is the most important diagnostic tool for venous ulcers. This noninvasive imaging test allows your vein specialist to assess blood flow, identify faulty vein valves, and determine whether venous reflux or obstruction is contributing to the ulcer. In some cases, additional circulation testing may be performed to rule out arterial disease before treatment begins.
Stages of Venous Leg Ulcers
Venous leg ulcers often develop gradually and progress through recognizable stages. Understanding these stages highlights the importance of early treatment.
Early Stage (Pre-Ulcer Changes):
Skin may become discolored, itchy, swollen, or tight around the ankles or lower legs. Conditions such as venous stasis dermatitis or lipodermatosclerosis may be present before an open wound develops.
Active Ulcer Stage:
An open sore forms, typically near the ankle. The ulcer may ooze fluid, cause discomfort, and heal slowly due to ongoing venous pressure.
Chronic or Non-Healing Stage:
Without treatment of the underlying vein disease, ulcers may persist for months or recur repeatedly. Chronic ulcers carry a higher risk of infection and complications.
Early diagnosis and intervention significantly improve healing time and reduce the risk of progression.
Compression Therapy
Compression therapy is a cornerstone of venous ulcer management and plays a vital role in improving circulation.
Medical-grade compression helps:
- Reduce swelling and venous pressure
- Improve blood flow back to the heart
- Decrease fluid leakage into surrounding tissues
- Support wound healing
Compression may include socks, wraps, or multilayer bandaging, depending on the ulcer’s severity and circulation status. Compression should always be prescribed and monitored by a healthcare professional, especially when arterial disease is a concern.
When used correctly and consistently, compression therapy significantly improves healing outcomes and helps prevent recurrence.
When to See a Vein Specialist
Early evaluation by a vein specialist can prevent complications and improve healing outcomes. You should seek specialized care if you experience:
- A leg ulcer that does not improve within 2–4 weeks
- Recurrent ulcers in the same area
- Increasing pain, swelling, or drainage
- Skin discoloration, thickening, or hardening of the lower legs
- A history of varicose veins, leg swelling, or prior ulcers
Prompt treatment of venous disease can significantly reduce healing time, lower the risk of infection, and help restore long-term leg health.
Why Choose Tennessee Vein Center for Leg Ulcer Treatment?
At Tennessee Vein Center, leg ulcer care is led by Keith E. Campbell, MD, a Knoxville native and highly experienced vein specialist who has dedicated his practice exclusively to the diagnosis and treatment of venous disease since 2003. Dr. Campbell is dual-board-certified and brings decades of focused expertise in treating complex venous conditions, including chronic and non-healing leg ulcers.
Our approach goes beyond wound care alone by identifying and treating the underlying vein disease responsible for ulcer formation and recurrence. With deep roots in East Tennessee and a long-standing commitment to the community, Tennessee Vein Center offers personalized, evidence-based care designed to promote healing, restore circulation, and support long-term leg health.
Effective Venous Ulcer Treatment Near Knoxville
If you or someone you know is dealing with venous ulcers, seeking specialized treatment in leg ulcers’ early stages is essential for effective management and healing.
At Tennessee Vein Center, we offer specialized treatment options for venous ulcers to address the root cause and promote healing.
Our team provides personalized care and advanced therapies to alleviate symptoms, improve circulation, and facilitate ulcer healing. Contact us today to learn more about our comprehensive approach to venous ulcer treatment and regain comfort and confidence in your vascular health journey.