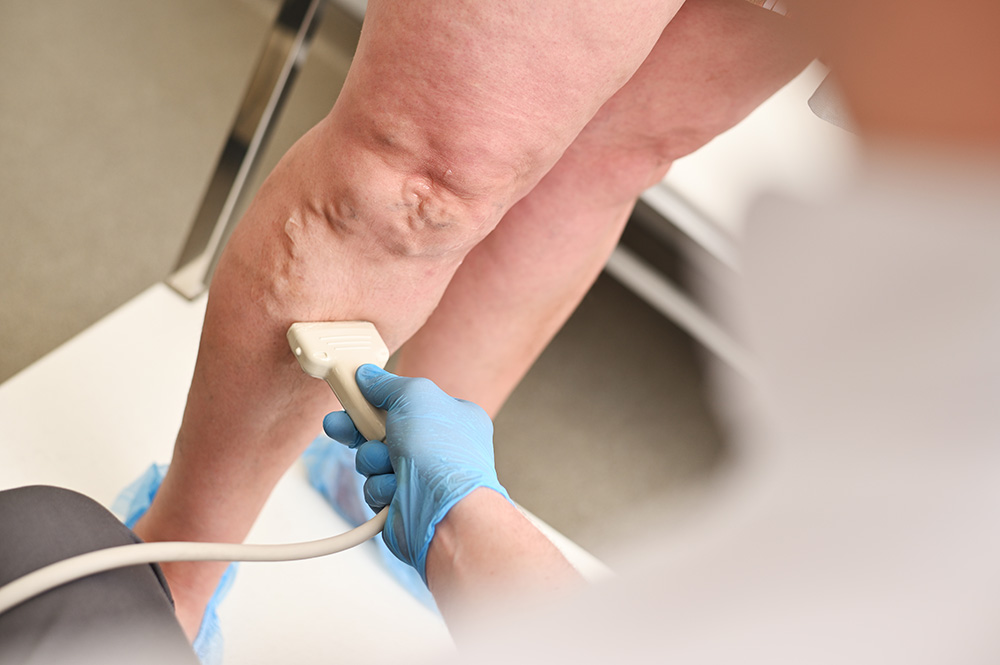
Vein Health and Aging: How to Protect Your Veins Over Time
Your veins work tirelessly every day, carrying blood back to the heart against gravity.
Over the years, however, they can become weaker and more vulnerable to damage, which is why vein problems often become more common with age.
From visible varicose veins to circulation issues that impact comfort and mobility, understanding how aging affects your veins is key to keeping them healthy for the long term.
In this blog post, we’ll explain the changes that happen with age, share prevention strategies, and show you when it’s time to seek professional care. Continue reading to learn more.
How Aging Affects Your Veins
As the years go by, your veins experience natural wear and tear that can affect how efficiently they move blood back to your heart.
Research published in the National Library of Medicine shows that with age, venous valves undergo structural changes, like thickening and the buildup of connective tissue, which make them less flexible and impair their function.
This reduced elasticity contributes to blood pooling and increased venous pressure, making conditions like varicose veins and chronic venous insufficiency more likely in older adults.
Understanding these changes can help you take proactive steps to protect your circulation and overall vascular health.
Common Age-Related Vein Changes
As you get older, your veins and their one-way valves naturally lose elasticity and strength. This makes it harder for them to push blood upward toward the heart, leading to increased pooling in the legs.
Other changes can include:
- Thinner vein walls that are more prone to stretching.
- Weaker valves that allow blood to flow backward.
- Slower healing in the legs and feet due to reduced circulation.
Why Do Veins Get Worse With Age?
Aging impacts multiple systems that support vein health:
- Collagen loss reduces structural support for vein walls and valves.
- Slower circulation means blood moves less efficiently, increasing leg pressure.
- Cumulative wear and tear from years of standing, walking, and other activities adds strain to the vascular system.
Lifestyle factors like diet, activity level, and medical history also play a role in how quickly veins weaken.
Signs of Vein Problems in Older Adults
If you notice any of the following symptoms of vein disease, it may be time to have your veins evaluated:
- Swelling in the legs, ankles, or feet.
- Aching, heaviness, or throbbing in the legs.
- Bulging, twisted veins visible under the skin.
- Skin discoloration or dryness around the ankles.
- Sores or ulcers that heal slowly.
Understanding the Most Common Vein Conditions
As we age, certain vein conditions become more likely due to natural changes in the vascular system.
Below are some of the most common issues that affect older adults and how aging influences their development.
Varicose Veins and Aging
Varicose veins are enlarged, twisted veins that develop when the one-way valves inside them fail to function correctly, allowing blood to pool in the legs.
This pooling increases pressure inside the vein, causing it to stretch and bulge.
With age, vein walls and valves naturally lose elasticity and strength, making it easier for varicose veins to form or worsen.
Older adults may notice more discomfort, swelling, and visible bulging veins over time, especially if other risk factors, like prolonged standing or a family history, are present.
Chronic Venous Insufficiency in Seniors
Chronic venous insufficiency (CVI), or vein disease, is a condition where the valves in the leg veins can’t keep blood flowing efficiently toward the heart.
This leads to ongoing pressure in the veins, which can cause swelling, skin changes, and even open sores.
In seniors, CVI is more common because years of strain on the circulatory system weaken the valves and vein walls.
Reduced mobility, age-related changes in blood vessel elasticity, and other health conditions can further contribute to the severity of CVI in older adults.
Spider Veins and Cosmetic Concerns
Spider veins are small, visible blood vessels that appear close to the surface of the skin, often in a web-like pattern.
While generally harmless, they can be a sign of increased pressure in the veins or early valve weakness.
As we age, skin becomes thinner and vein walls more fragile, making spider veins more noticeable.
Older adults may find these veins more common, especially in the legs and ankles, and while they’re often cosmetic, they can signal underlying circulation issues that may require attention.
Tips to Keep Veins Healthy As You Age
Even though aging is a natural risk factor for vein problems, adopting healthy habits can make a big difference in keeping your circulation strong.
Focus on daily choices that support vein function, reduce pressure in the legs, and maintain mobility:
- Stay physically active with low-impact exercises like walking, swimming, or cycling.
- Elevate your legs when resting to help blood flow back toward the heart.
- Wear compression stockings if recommended by your healthcare provider.
- Maintain a healthy weight to prevent extra strain on your veins.
- Drink plenty of water and eat a diet rich in fiber, antioxidants, and healthy fats.
Making these habits part of your routine can help protect your veins and reduce the risk of discomfort or complications.
Preventing Vein Problems With Age
Prevention is about consistency. Over time, small changes in your daily routine can protect your veins from unnecessary stress:
- Avoid sitting or standing in one position for long periods.
- Stretch and move your legs every 30–60 minutes.
- Choose supportive shoes that promote good posture and circulation.
- Manage chronic conditions like diabetes, high blood pressure, or high cholesterol, which can all impact vascular health.
By combining these preventive steps with regular check-ins on your vein health, you can stay ahead of potential issues as you age.
When to See a Vein Specialist
Don’t ignore symptoms that could point to vein disease. Seek an evaluation if you experience:
- Leg swelling, aching, or heaviness.
- Bulging, twisted veins visible under the skin.
- Skin discoloration or dryness around the ankles.
- Sores or ulcers on the legs that heal slowly.
Early intervention can help prevent complications, improve your comfort, and maintain your mobility.
At Tennessee Vein Center, we offer thorough assessments to identify the cause of your symptoms and recommend the most effective vein treatment for your needs.
Why Choose Tennessee Vein Center for Senior Vein Care
Aging veins require specialized attention, and that’s exactly what we provide.
Our team combines advanced diagnostic tools with minimally invasive vein treatments tailored to your needs and lifestyle.
We also offer guidance on long-term strategies to maintain healthy circulation, helping you stay active and comfortable at every stage of life.
When it comes to protecting your vein health as you age, you deserve expert care and a personalized approach. We’re here to help you take the next step toward healthier legs and a better quality of life.
Contact us today to learn more.